BAL Leading the Way Series
Remember when we used to watch Captain Kirk talk into his chirping communicator and order Scotty to beam him up? And what about that handy medical scanner the size of a pack of cards that Dr. McCoy waved around to assess and diagnose his patients in the starship’s sick bay? We may now all have smartphones to stay in constant touch with each other, but outside of a state-of-the-art hospital with multi-million-dollar scanners and MRI machines, we are still some years away from the Star Fleet’s instantaneous medical technology, right?
Wrong.
Advances in our ability to gather real-time information on the human body are poised to revolutionize not just how we diagnose diseases, but make dramatic, life-altering, positive impacts on the critical timeline for diagnosis and treatment by detecting a disease event before symptoms occur. And Bay Area Lyme is leading the way by investing in research that will further illuminate our understanding of how—in real time—a Lyme infection impacts the human body through the data collected by wearable technologies.
 You’re probably thinking, “But hold on, FitBits® and Apple® watches and other wearables have been around for a few years now, able to monitor our basic body functions, so this isn’t “new” news, is it?” Good point—and it’s a bit of yes, but a big dollop of no, too.
You’re probably thinking, “But hold on, FitBits® and Apple® watches and other wearables have been around for a few years now, able to monitor our basic body functions, so this isn’t “new” news, is it?” Good point—and it’s a bit of yes, but a big dollop of no, too.
Here’s the “new” and exciting part: machine learning and artificial intelligence have become so sophisticated, we now have the technology to perform millions of checks daily on a person’s body, assessing moment-by-moment functionality. This means we can gather masses of data to map an individual’s health baseline and—as soon as data deviates from that baseline – we have robust quantitative evidence to flag a potential problem.
We now have the technology to perform millions of checks daily on a person’s body to gather masses of data to map an individual’s holistic health baseline and—as soon as data deviates from that baseline—we have robust quantitative evidence to flag a potential problem.
So, how does this relate to Lyme disease?
 Enter Michael Snyder, PhD, Chair, Dept. of Genetics and Director, Center for Genomics and Personalized Medicine, Stanford University, and the recipient of a Bay Area Lyme grant to fund an exciting study that explores how wearable technology can help measure and flag when an infection has been detected before symptoms emerge, or if serious health event is imminent. It can also measure what is happening while that health event is underway.
Enter Michael Snyder, PhD, Chair, Dept. of Genetics and Director, Center for Genomics and Personalized Medicine, Stanford University, and the recipient of a Bay Area Lyme grant to fund an exciting study that explores how wearable technology can help measure and flag when an infection has been detected before symptoms emerge, or if serious health event is imminent. It can also measure what is happening while that health event is underway.
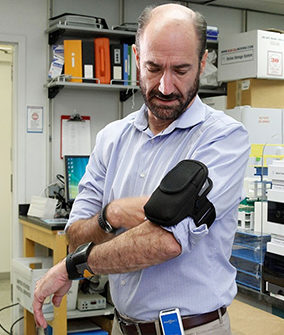
Dr. Snyder is something of a wearables fanatic, by his own admission. His passion is using technological advances in concert with genomes to not only understand the function, evolution, mapping and editing of human DNA, but to invent technologies that will illuminate—instantly—what’s working, what’s not, and what’s potentially an early warning of a serious problem in your body. And his connection to Lyme is personal.
“I’d been building a fence on my brother’s property in rural Massachusetts. I knew that infected ticks were a big issue, so I was already alert to Lyme. I was monitoring myself using state-of-the-art wearables that a company we are invested in had developed, but everything seemed fine.”
Two weeks later, Snyder was on a plane traveling to Norway. During the flight he noticed that his wearable monitoring device was registering an elevated heart rate and a significant reduction in blood oxygen levels. “Being on a flight can raise your heart rate, so I wasn’t unduly concerned. With wearables, you always have to contextualize the data,” notes Snyder, “But after I landed and had been in Norway for a couple of days, I noticed that my heart rate and blood oxygen levels never returned to my normal baseline. I suspected a new, underlying infection. I immediately thought of Lyme.”
Concerned, Snyder saw a Norwegian doctor who was initially skeptical. However, the doctor agreed to perform blood tests and—bingo! Snyder’s blood work returned positive for Lyme. Snyder started a course of doxycycline immediately and, on his return to the US continued treatment and close monitoring.
“What’s amazing about my personal experience is this: before the fence-building project, I had just recently donated blood. During that screening, I knew that I did not have Lyme and I can prove this from those serology results. So, I can trace the timeline exactly from being uninfected, to being infected, noticing the shift in my baseline data as I was able to monitor my body so closely, and then acting immediately on the information that led to an early diagnosis, treatment and cure.” Snyder had no other symptoms of an acute Lyme infection—including no evidence of an erythema migrans (EM) rash—so without the wearables flag, he could have gone significant time before discovering the infection, by which time the disease could easily have taken hold and been much harder to treat.
“I can trace the timeline exactly from being uninfected, to being infected with Lyme, noticing the shift in my baseline data as I was able to monitor my body so closely, and then acting immediately on the information that led to an early diagnosis, treatment and cure,”
– Michael Snyder, PhD
 What’s exciting about Dr. Snyder’s work is that this not only has positive ramifications for diagnosing and treating early Lyme disease, but it can also help those with chronic/persistent Lyme infections, too, by mapping a person’s regular baseline and then measuring the body’s response when deviations occur. This is key for those who are trying to manage their long-term Lyme symptoms and could be cross-checked to other data like a food diary, for example, to help illuminate other variables that can compound or alleviate symptoms.
What’s exciting about Dr. Snyder’s work is that this not only has positive ramifications for diagnosing and treating early Lyme disease, but it can also help those with chronic/persistent Lyme infections, too, by mapping a person’s regular baseline and then measuring the body’s response when deviations occur. This is key for those who are trying to manage their long-term Lyme symptoms and could be cross-checked to other data like a food diary, for example, to help illuminate other variables that can compound or alleviate symptoms.
Lyme patients and others with chronic/persistent symptoms typical of Long-haul Covid, chronic fatigue syndrome and chronic/persistent Lyme often experience extended periods of fatigue, known as “crashes,” and wearables are a powerful way that researchers could better understand these debilitating episodes. “Participants are currently being enrolled into the Crash Course study, funded by a grant from Bay Area Lyme Foundation, and we are actively seeking more participants. It would be ideal to have up to 1,000 persistent Lyme patients involved,” according to Dr. Snyder. “As we seek to understand the body’s response to tick-borne diseases and other infections, the more data we can collect, the more we can untangle the mysteries around how the immune system works to tackle threats like persistent Lyme and Long Covid.”
The Crash Course study aims to understand why crashes occur, the differences in crashes between and within individuals, and ultimately how to predict and prevent crashes using wearable devices.
As we look ahead, it’s abundantly clear that using wearable technology to map people’s baseline health status and catch infections before the onset of symptoms, or use wearables to monitor those with chronic/persistent conditions will completely transform the way patients are diagnosed and treated. By collecting precise, real-time data in a customized way, we are truly on the brink of solving some of the most intractable challenges facing human health management going forward. And in ways that are convenient, non-invasive and affordable. The future of healthcare truly is now. We think Captain Kirk and Dr. McCoy would definitely approve.
This Bay Area Lyme Foundation blog is part of our BAL Leading the Way series and is based on a conversation between Wendy Adams, Bay Area Lyme Foundation Research Grants Director, and Dr. Michael Snyder, Stanford W. Ascherman Professor and Chair, Department of Genetics Director, Center for Genomics and Personalized Medicine Stanford University recorded in July 2021. Dr. Snyder is a major participant in the ENCODE project, the public research project that aims to identify functional elements of the human genome. He authored the book: Genomics and Personalized Medicine: What Everyone Needs to Know. He is also a cofounder and a board member of several biotechnology companies. You can access a recording of their extended conversation as either a podcast or video.
To be eligible for the Crash Course study, you must be at least 18 years old, experience fatigue episodes or “crashes” that persist for at least 24 hours, and have been diagnosed with Long-haul COVID-19, chronic Lyme, or ME/CFS. People with chronic Lyme who have also been diagnosed with COVID-19 may also participate in the study. To find out if you are eligible for the study, please email the study coordinator to let them know your interest at crashcoursestudy@stanford.edu. The study coordinator will contact you within 2–3 weeks of receiving your email.
 Ticktective™ Podcast Series
Ticktective™ Podcast Series
Ticktective™ podcast, a Bay Area Lyme Foundation program, investigates the latest scientific knowledge and advances in Lyme and tick-borne diseases, and offers insightful discussion with researchers, physicians, patients, and thought leaders in the field. Wendy Adams, Bay Area Lyme grant director, interviews Dr. Snyder in the podcast “Genomics and Personalized Medicine: What Everyone Needs to Know“.

