 On March 2nd, Bay Area Lyme again hosted another of its Speaker Series events. These popular salon-style events allow community members to come together in an intimate forum to share stories and hear directly from experts in the field.
On March 2nd, Bay Area Lyme again hosted another of its Speaker Series events. These popular salon-style events allow community members to come together in an intimate forum to share stories and hear directly from experts in the field.
The featured speakers this time were Dr. Christine Green, MD, a recognized leader in Lyme disease diagnosis and treatment and Allie Cashel, author of Suffering the Silence: Chronic Lyme Disease in an Age of Denial. Both shared personal and professional perspectives on the challenges of diagnosing Lyme disease.

Dr. Green has practiced integrative and orthomolecular medicine since opening her private practice in the Bay Area in 1983. Her focus is on chronic fatigue, chronic pain, and tick-borne diseases and she leverages lifestyle adjustment, natural and bio-identical nutrients, and pharmaceuticals in treating her patients. Dr. Green is also on the board of ILADS, the International Lyme and Associated Disease Society, where she serves as Director of Education, and on the board of LymeDisease.org (formerly CALDA).
Tick-borne diseases are challenging, acknowledged Dr. Green. Less than a third of all patients bitten ever see the tick and as few as 20% of those infected actually see a recognizable rash. There is far too little understanding much underdiagnosis.*
Tick-borne pathogens are stealth pathogens: the incubation period may be indeterminate — symptoms can develop at various times post inoculation, escalating aggressively after a period of seeming remission; infections may present indolent or asymptomatic carriage — symptoms often appear subtle or viral like; and the bacteria has developed sophisticated adaptations for evading the natural immune system allowing for the bacteria and related infection to become virulent — even once the immune system makes a specific antibody to Lyme, it does not guarantee eradication, because Lyme can change its “coat.”
Lyme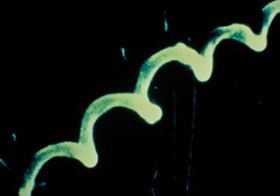 , in particular, is especially potent — it has a little flagella and can swim through vessel wells, travel inside of cells, or hang out in lymph tissue affecting the brain and nerves, tendon and joint linings, heart muscle, lymph nodes, the urinary tract, liver, and gastrointestinal system.
, in particular, is especially potent — it has a little flagella and can swim through vessel wells, travel inside of cells, or hang out in lymph tissue affecting the brain and nerves, tendon and joint linings, heart muscle, lymph nodes, the urinary tract, liver, and gastrointestinal system.
Bartonella infects blood vessels and cells and can go straight to any tissue as a result. Babesia infects red blood cells, potentially traveling to just about any body tissues and Ehrlichia and Anaplasma invade white blood cells, thus deactivating the immune system.
Untreated, Lyme and all tick-borne diseases have the potential to wreak havoc on one’s health. Dr. Green talked specifically about some of the highly debilitating presentations of late stage persistent Lyme disease including neurological, neurocognitive, and neuropsychiatric issues caused by nerve cell death, inflammation and swelling, and cytokine release; gastorintestinal manifestations, particularly common in children; rheumatological symptoms due to inflammation of the joint linings and fluid; and cardiovascular issues including pericarditis and myocarditis.
The challenge, Dr. Green explained is that these type of symptoms are not consistent, specific, or exclusive to the individual pathogens to facilitate diagnosis. And primary care physicians who are graded on efficiency (minimal time spent with patients — Kaiser doctors reportedly get just 8 minutes!) and accuracy (their ability to “name” and pass on the diagnosis to an appropriate specialist) are not equipped to explore and investigate the many signs and signals of an evasive infection like Lyme disease. Often a patient is quickly assessed with a particular diagnosis (say gastroenteritis), then passed onto a specialist who may rule out the initial assessment but then passes the patient onto another specialist to evaluate seemingly unrelated symptoms (maybe a rheumatologist to evaluate the possibility of fibromyalgia or chronic fatigue). What gets lost is the potential for pattern recognition and a more holistic evaluation of the patient’s medical history and symptoms. And even if accurately diagnosed, successful treatment usually requires an integrative approach that focuses on both internal and external factors (infections, toxins, and stressors), that many doctors simply don’t have the capacity to provide.
“It is important for doctors to become more familiar with the experience of Lyme patients and more versant on the myriad of symptoms that Lyme can present,” argued Dr. Green. “Lyme disease is here. You only need look to the ecology study in Bay Area parks that Bay Area Lyme Foundation funded last year to see that,” she explained, further challenging that perhaps the results needed to be shared with every doctor and veterinarian in the area. Dr. Green’s talk was brought to life with compelling case studies highlighting the challenges of diagnosis and treatment, leaving everyone with a sense of urgency and greater understanding.
Dr. Green also reiterated the need for every individual to self-advocate and emphasized some important things to keep in mind, particularly here in the Bay area:
 Not everyone sees a tick or a rash. If you have any symptoms, you need to discuss with your doctor. You also want to track symptoms. The bacteria can live quietly and multiply, reappearing at a later date with new virulence and/or different symptoms.
Not everyone sees a tick or a rash. If you have any symptoms, you need to discuss with your doctor. You also want to track symptoms. The bacteria can live quietly and multiply, reappearing at a later date with new virulence and/or different symptoms.- The most “dangerous” animal as far as Lyme is concerned is the squirrel: 8 out of 10 grey squirrels, the ones you see in your backyard and every other public space, carry Lyme. Children and pets are typically most exposed whether on soccer fields and playgrounds or in the woods and on hikes.
 The most dangerous vegetation is Oak chaparral, the dense shrubland native to the coastal areas of California from San Francisco Bay area down to Tijuana. These areas have higher tick density.
The most dangerous vegetation is Oak chaparral, the dense shrubland native to the coastal areas of California from San Francisco Bay area down to Tijuana. These areas have higher tick density.- March to July is the most dangerous time though recent climate fluctuations and our mild winters here in the bay area mean that there is risk virtually year round.
- It is critical to tick-check – Shed clothes when you come inside, take a shower, wash gear, wash hair (especially longer hair) …
- Best recommendation for first aid? In general, soap and water. Remove the entire tick, put in plastic bag with a bit of moisture.** Treat with Neosporin if there is a puncture to skin.
Allie Cashel, whose book, Suffering the Silence, chronicles the stories of patients suffering from chronic Lyme disease in the US and beyond, has received much acclaim for her “sensitive, human look at the illness and the struggle patients face in finding recognition and treatment.” Allie knows the situation well, having finally been diagnosed with Lyme disease many years after its symptoms first emerged and only with the persistence of pushing through dismissal from many healthcare professionals despite the fact that both her father and her three siblings also were diagnosed with Lyme. The book, which started out as a research project while at Bard College also became a passion project and an opportunity to help “change the thinking about Lyme disease” — she hopes that by sharing more of the stories, patients, healthcare providers, and the public will come to recognize the scope of the epidemic and the dangers of dismissal.

The evening concluded with an energetic Q&A session in which the experts addressed issues such as climate change, geographic and demographic patterns in Lyme risk and infection incidence, and new developments and options for treatment.
For more information about the next Speaker Series event, scheduled for June 1, please click here.
—————————
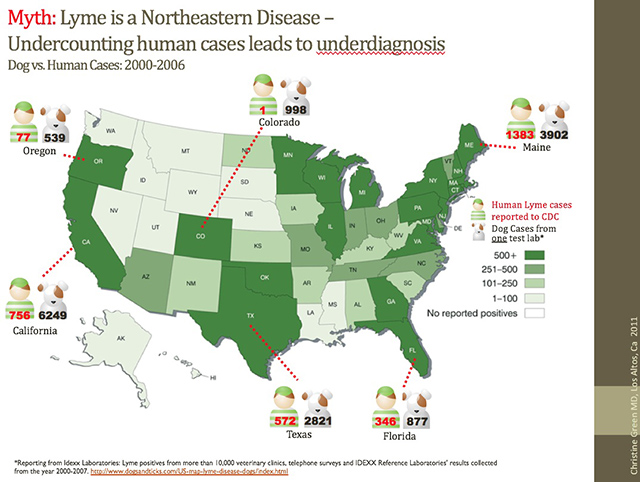
*Dr. Green presented some compelling data presenting correlation between dog and human cases of Lyme disease indicating potentially substantial levels of underreporting in many areas outside of the northeast.
**Note: It is always wise to save the tick if possible. You can have the tick tested for Lyme disease if you experience symptoms and tick-testing is highly accurate (unlike human diagnostics). Bay Area Lyme Foundation is now offering free tick-testing. Click here for more information about tick-testing.